In a review, Naheed Arfin Borah and Mamatha M. Reddy investigate how aurora kinases sit at the crossroads of two challenging cancer problems, pointing to them as possible therapeutic targets.
In 1971, physician and geneticist Alfred Knudson published a 4-page research paper that revolutionized the field of cancer genetics. Based on a statistical analysis of 48 cases of retinoblastoma-a rare childhood eye cancer-Knudson predicted the existence of tumor suppressor genes (TSG; genes that prevent cells from dividing nonstop). Fifteen years later, the first such gene was identified: the retinoblastoma (RB1) gene. It encodes the retinoblastoma protein (pRB), a key regulator of the cell cycle which restricts uncontrolled cell growth. Mutations in RB1 result in abnormal cell proliferation that leads to cancers such as small cell lung cancer, osteosarcoma, and retinoblastoma, among others. Yet more than fifty years after its discovery, treating cancers associated with the inactivation of tumor suppressor genes remains a challenge.
Cancer drugs are designed to inhibit proteins that drive tumor growth. But pRB is the opposite-it is a molecular ‘brake’. RB1 mutations remove this crucial curb, causing cells to divide continuously, resulting in cancer. This loss of pRB should trigger cell-death, but cancerous cells over-express cell cycle regulatory proteins called Aurora Kinases (AURKs) to suppress cell-death triggers. Excess AURKs, particularly, AURKA stabilizes the oncogene MYCN, which stimulates tumor growth in several childhood cancers. Similar to TSG loss of function, targeting MYCN has also been proven difficult due to its disordered structure. Can cancer drugs that block Aurora Kinases restore cell-death in both these instances?
In a review published in Current Cancer Drug Targets, Naheed Arfin Borah a postdoctoral fellow at University of Minnesota and Mamatha M. Reddy from LVPEI examine the current evidence for aurora kinases as potential therapeutic targets for these cancers. The authors report that blocking AURKs creates a phenomenon called ‘synthetic lethality’, where a cancer cell survives on a backup system but dies when that backup is removed. The review explores this across eight cancers-small cell lung cancer, osteosarcoma, triple-negative breast cancer, prostate cancer, retinoblastoma, neuroblastoma, rhabdomyosarcoma, and medulloblastoma.
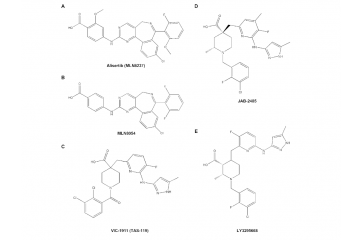
In many of these cancers, either RB1 loss or MYCN dysregulation decides the dependency on AURKs. Retinoblastoma is one cancer where both mechanisms occur — RB1 loss is often accompanied by MYCN dysregulation, creating a ‘feed-forward loop’ in which MYCN increases the expression of AURKA, which in turn stabilizes MYCN. The review also examines several AURKA inhibitors currently in clinical trials and newer molecules called PROTACs that degrade AURKs. Early results seem promising.
‘What makes aurora kinases interesting is that many tumors appear to depend on them once key safeguards like RB1 are lost. That creates a potential vulnerability which if we can target, we may be able to selectively affect cancer cells while sparing normal cells,’ said Naheed Arfin Borah along with Mamatha Reddy, Research Scientist, LVPEI.
Citation
Borah NA, Reddy MM. Aurora Kinases as Potential Therapeutic Targets for Tumors with pRB and/or MYCN Dysregulation. Curr Cancer Drug Targets. 2026 Jan 8. doi: 10.2174/0115680096395779251022060212. Epub ahead of print. PMID: 41540536.
Photo credit: Figure 5, Borah et al.