Biomaterials for Dry Eye Disease
Written by Yamini Joshi
Published 22nd February 2023
A review paper by Dr Swati Singh and others from the L V Prasad Eye Institute explores the use of biomaterials for drug delivery in dry eye disease (DED) research and discusses the development stage they are in.
Dry eye disease (DED) is an ocular surface disease with tear film instability, leading to inflammation and damage to the eye’s surface. DED is a chronic condition that causes constant discomfort, disrupts daily function, and in its severe form, even leads to vision loss. DED symptoms are addressed using topical ophthalmic solutions such as lubricating eye drops, anti- inflammatory agents and immunosuppressive drugs depending on disease severity. However, such topical solutions can only address the symptoms and must be applied for life. Their long-term use can lead to side effects that include cataract and glaucoma. The fundamental limitation of conventional ophthalmic solutions is their limited bioavailability, due to the eye’s natural tear drainage mechanisms and require their constant re-use.
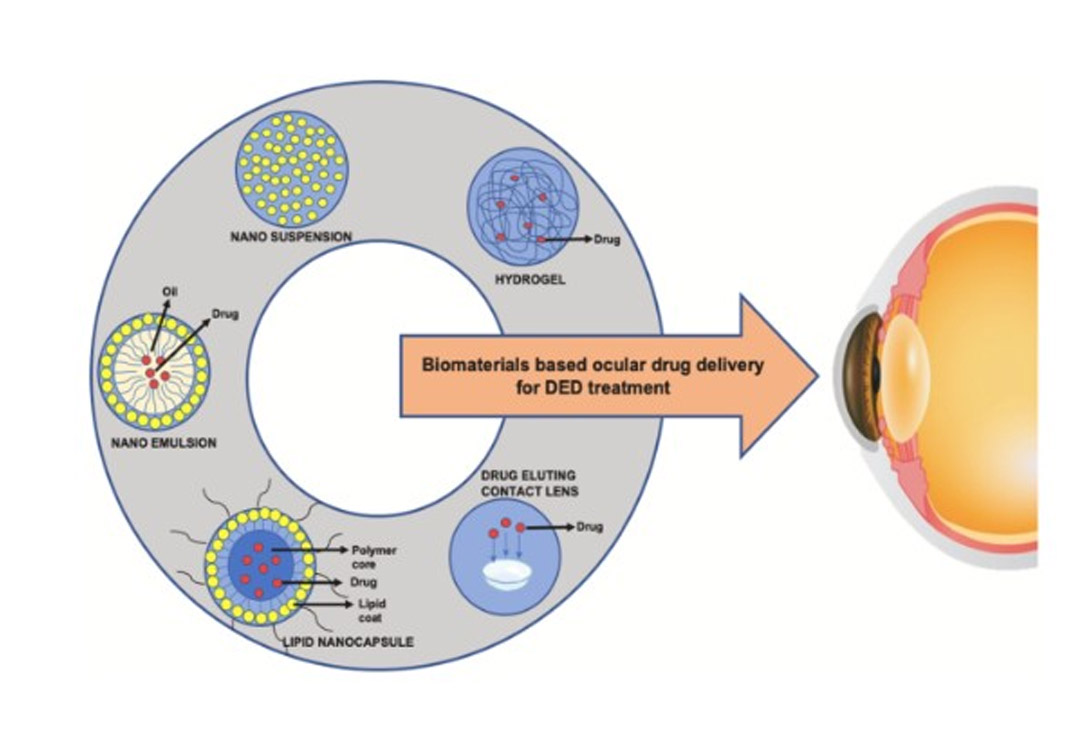
A variety of biomaterials like nano systems, hydrogels, and contact lenses promise longer bioavailability with steady dosage on the ocular surface. Several teams are exploring the safety and efficacy of biomaterials in animal models and are only now addressing their potential in human trials. A variety of biomaterial technologies offer a range of choices ranging from drug-elution, delayed release, osmolarity or charge to restore homeostasis on the ocular surface. They vary in design, efficacy and use, and are at different stages of development.
A review in the Experimental Eye Research by Dr Swati Singh and others analyzed the published studies on biomaterials for tackling dry eye disease. The paper looks at a range of nano systems, hydrogels and contact lenses, and discusses their current state of development. These biomaterials are used to package and release lubricants and anti-inflammatory drugs over extended periods at a sustained cadence.
Nano systems like nanoparticles, lipid molecules, nanowafers, nanogel and nano emulsions are widely studied biomaterials to treat DED. Each material is best suited to deliver specific drugs and to target a particular aspect of DED treatment, such as increased tear production, volume, or stability; reduced inflammation; or longer retention. Hydrogel-based drug delivery systems are also discussed, with particular attention to their unique ability to respond to changes in temperature, pH and charged states. Hydrogel patches are beginning to see human trials. Hydrogel or silicone hydrogel-based contact lenses with different drug loading and delivery methods have a long history of DED-related research, the paper notes. However, all these systems need extensive research before their commercial availability to treat DED.
‘DED is a very common health problem, and the treatment is only palliative. Patients need eye drops every few hours, throughout the day adding to compliance issue and more preservative related side-effects. Biomaterials are like a sponge, if drugs are inside the sponge, it slowly releases the drugs and reduces the frequency of the drug administration. While they offer numerous advantages, more long-term studies are needed before regulatory approval can be obtained and biomaterials are commercially available for DED patients,’ says Dr Swati Singh, Assistant Ophthalmologist, Centre for Ocular Regeneration, LVPEI
Citation
Thacker M, Singh V, Basu S, Singh S. Biomaterials for dry eye disease treatment: Current overview and future perspectives. Exp Eye Res. 2023 Jan;226:109339. doi: 10.1016/j.exer.2022.109339. Epub 2022 Dec 5. PMID: 36470431.
Photo credit: Various drug delivery systems for DED treatment; Thacker et al.