Keratoconus Management by Indian Ophthalmologists
Written by Tejah Balantrapu
Published 24th October 2023
A research team from LVPEI consisting of Drs Rashmi Deshmukh, Pravin Krishna Vaddavalli, and Alok Srivastava reports on the current trends in diagnosis and treatment procedures for keratoconus management among Indian ophthalmologists.
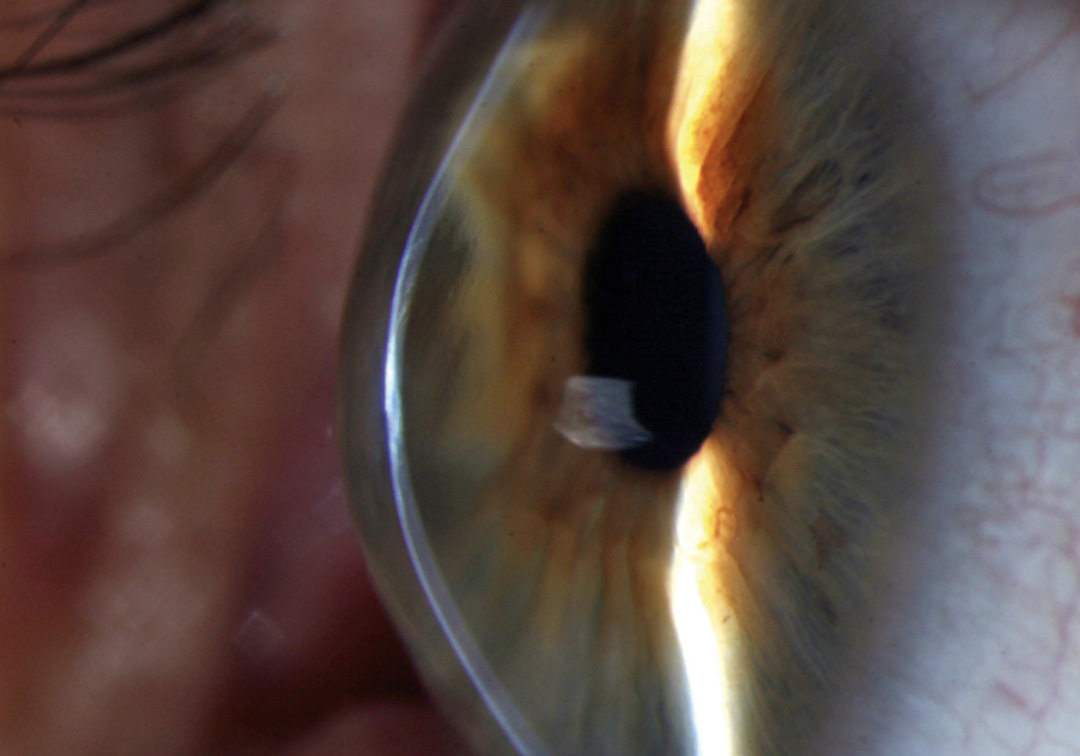
The cornea is a clear, dome-shaped layer in the front of the eye. Keratoconus is a condition where the cornea thins and elongates, progressively protruding outward into a cone-like shape. This gradual thinning causes the cornea to become distorted, leading to increased loss of visual acuity and quality. The onset of keratoconus is often seen in teenagers and the corneal bulging usually reduces by the time they are in their 30s. Because it primarily affects youngsters and is irreversible, early diagnosis of this condition is crucial for its effective management.
Diagnostic technologies that monitor and map the development of keratoconus have come a long way in the last 30 years. We have progressed from tools for corneal topography, which create a 2D image of the cornea’s surface, to newer tomographic tools that can generate a 3D image of the whole cornea. A similar leap in treatment options has led to non-surgical interventions like corrective spectacles or contact lenses and minimally invasive procedures like corneal collagen crosslinking (CXL) that halt keratoconus progression at an early stage. CXL involves using vitamin B12 drops and UV rays to crosslink corneal collagen fibres, stiffening the cornea and preventing it from coning any further. So, what diagnostic and treatment strategies do Indian ophthalmologists prefer for keratoconus management?
In a new cross-sectional, survey-based study published in the Indian Journal of Ophthalmology, Drs Rashmi Deshmukh, Pravin Krishna Vaddavalli, and Alok Srivastava investigated the keratoconus diagnosis and treatment patterns prevailing among ophthalmologists in India. Of the 273 participating Indian ophthalmologists, 41% were fellowship-trained cornea specialists while 33% had over 15 years of experience. 92% of all participants indicated mapping corneal tomography as an essential test in keratoconus diagnosis. CXL was a popular treatment choice, with half of the participating ophthalmologists noting their preference for the procedure on corneas of at least 400-micron thickness. In situations where CXL was not possible, more than half (55%) of the ophthalmologists prescribed corrective contact lenses, while others recommended surgical options like cornea transplant (35%).
Keratoconus can lead to loss of visual acuity, so, combining CXL with refractive surgery can improve spectacle‑corrected visual acuity. Yet, half (50.55%) of the ophthalmologists did not go for surgical options like photorefractive keratectomy (PRK) or intracorneal ring segment (ICRS) implantation. Among the 49 ophthalmologists who were comfortable performing both PRK and ICRS with CXL, 53% (26) were fellowship-trained specialists and 35% (17) had over 15 years of experience. Increasing the number of training fellowships could elevate the baseline experience among Indian ophthalmologists leading to improved outcomes in keratoconus treatment.
‘There is a need for standardising the practice patterns among various ophthalmologists involved in keratoconus management,’ concludes Dr Rashmi Deshmukh, consultant ophthalmologist at LVPEI, and the corresponding author of this paper. ‘Fellowship training and knowledge of the existing treatment options would help in better visual outcomes.’
Citation
Deshmukh R, Shrivastava AK, Vaddavalli PK. Prevailing practice patterns in keratoconus among Indian ophthalmologists. Indian J Ophthalmol 2023;71:3229-34.
Photo credit: Keratoconus; by David Yorston, Community Eye Health Journal; CC BY 2.0.