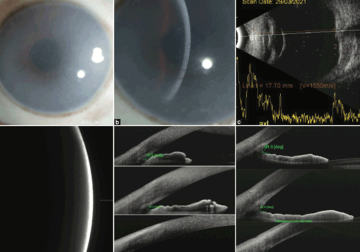
A study by Dr Muralidhar Ramappa and others from L V Prasad Eye Institute evaluated the use of anterior segment morphometry to assess any changes in patients with mucopolysaccharidoses (MPS). It highlights the value of correlating anterior segment changes to disease progression and the early diagnosis of glaucoma in people with MPS.
Mucopolysaccharidoses (MPS) are rare, metabolic life-limiting disorders caused by the absence or malfunction of certain enzymes in the body. People with MPS cannot break down certain accumulated sugars in their body’s cells and tissues. This causes various cognitive and musculoskeletal defects, including ocular manifestations such as corneal clouding and glaucoma. MPS is classified into four types (Type I, II, IV and VI), with an estimated prevalence of 2 to 6 per 100,000 births.
Recent advances in treatment modalities have shown promise for reversing systemic problems in the body, but they fail to address MPS’ damage to the eye. In fact, children with MPS require close follow-up as they grow into adulthood in case they need urgent intervention to save their sight. MPS (excluding type II) leads to corneal clouding in the child’s first year itself. It also seems to impact the eye’s axial length. Even less under-reported is the prevalence of secondary glaucoma, either due to corneal thickening or unnatural deposits of sugars in the eye. Assessing these anterior segment alterations may provide answers for diagnosing early onset glaucoma in children with MPS.
A new study in the Indian Journal of Ophthalmology by Dr Muralidhar Ramappa and others from the L V Prasad Eye Institute evaluated the use of anterior segment morphometry to assess changes in the ocular morphology in patients with MPS and to explore whether these measurements correlate with an early diagnosis of glaucoma. The study compared a cohort with MPS to age-matched healthy controls, 35 eyes each, with a total of 70 eyes (of 35 children), mostly male (71%). The study included a comprehensive eye examination to measure refraction and anterior segment imaging to note corneal clouding, central corneal thickness (CCT), intraocular pressure (IOP) anterior chamber depth (ACD), and axial eye length (AXL).
The study found that children with MPS recorded abnormal eyeball growth, higher corneal thickening, and loss of corneal transparency. The study also found secondary glaucoma and optic nerve involvement—in fact 28% of their MPS patients had glaucoma, far higher than the reported 2-10% in previous studies. A key insight of the study is the association between architectural changes to the anterior segment of the eye and disease progression including secondary glaucoma. Incorporating eye exams into MPS standard of care can lead to an improvement in the quality of life of these patients.
‘Regular eye exams are essential to standard of care for patients with MPS. These exams can help detect eye problems early and prompt treatment to prevent vision loss,’ says Dr Muralidhar Ramappa, Faculty Ophthalmologist, Institute for Rare Eye Diseases & Ocular Genetics, LVPEI. ‘The high childhood mortality in MPS has directed much of the research on the life-threatening outcomes of the condition, rather than ocular symptoms and manifestations. This paper underscores the value of correlating anterior segment changes to disease progression.’
Citation
Ramya Achanta DS, Mohamed A, Chaurasia S, Senthil S, Mandal AK, Takkar B, Mishra DK, Edward DP, Ramappa M. Objectively measuring anterior segment alterations in the eyes of mucopolysaccharidoses: Its utility in early diagnosis of glaucoma. Indian J Ophthalmol. 2022 Dec;70(12):4180-4185. doi: 10.4103/ijo.IJO_1300_22. PMID: 36453310.